Report on new eye service at Mulanje Mission Hospital
Andrew Feyi-Waboso updates us on his progress in Malawi on his recent trip from January to March 2023.
As we conclude our visit to Mulanje Mission Hospital, Malawi Cyclone Freddy has already left devastation and laid waste so many lives in its wake. It is sad to leave just as we are getting into gear and into some kind of flow but I take consolation that the good work started will continue.

Setting up and seeing patients
The new unit is a welcome addition to a busy mission hospital. There were some delays with the contactor handing over the unit. Setting up the equipment, testing and demonstrating to staff
how to use the equipment was a major milestone. Our first eye patients were seen on January 23rd. The combined Eye, Rehab and Dental unit was formally opened on 2nd March. Dignitaries and stake holders from far and near were in attendance. It was an opportunity to spread the news that these new services were available in the locality. Previously patients had travelled far to access services. Radio and TV interviews were made locally to inform the community about the new eyes and rehab Centre. We finished out last week on a high operating on 2 days of the week. Despite the 3 weeks of national mourning on account of Cyclone Feddy and the hardship patients came for cataract and glaucoma laser surgery.
In addition to our dedicated eye nurses we trained the rehabilitation staff Sally and Eunice in basic eye assessment. This included how to undertake a visual assessment, pupil examinations, keratometry and biometry. This means that in busy periods other staff can be called in to help-a unique partnership. A major achievement was getting the staff to gel together and work as a team. The nursing staff Michael Bridget and Kelly were very keen to learn. I was able to give tutorials every week to ensure they were confident in basic eye assessment. Our Monday morning 8am sessions was an opportunity to receive feedback, plan for the week and teach.

Collaborating with Zomba Eye unit
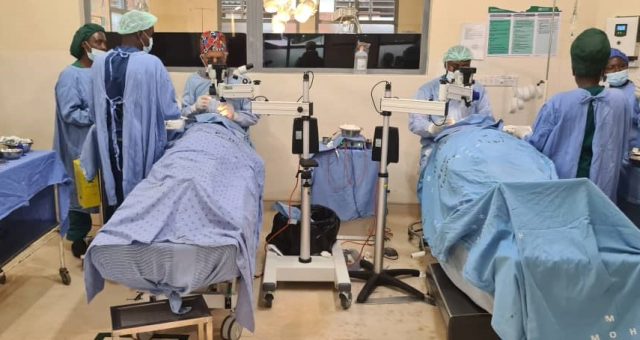
Before we started cataract surgery at Mulanje Mission Hospital our nurses were sent to Zomba Eye unit for training in intraocular operative theatre technique and giving local anaesthetic eye blocks. This training was timed to occur just before the joint surgery sessions held over 3 days at MMH when we were joined by Cataract surgeon from Zomba Owen Kanazawa and team. This ensured their new taught skills were tried out and tested. To increase throughput we operated on twin operating theatre tables in Theatre 2. Jointly 19 cataracts were done. As this was a teaching and learning session the emphasis was on learning rather than numbers operated on. Both teams had fun together doing intra-ocular surgery in the new eye unit. We concluded with a debrief so both teams were able to share the experience of learning and teaching together. This collaboration greatly enabled us proceed after they had left. We are so grateful to Dr Chinsisi Nyerenda and team atZomba Central Hospital eye unit for supporting us in this way.

Outpatients was busy with quite a diverse number of patients attending including children. Apart from cataracts other pathology seen included advanced glaucoma, diabetic retinopathy, a baby with congenital cataracts and a young patient with probable conjunctival squamous cell cancer. Sadly most patients presented with advanced disease. We also saw patients who had come over the border from Mozambique where eye services are extremely rudimentary.
No patient was turned away because they couldn’t pay for treatment . The initial cataract surgeries were all free. Patients for subsequent procedures were asked to make a contribution no matter how small.
Activity
By 22 March we had performed 45 eye procedures including 31 cataract operations (MSICS), five excisions of conjunctival lesions, 5 cyclodiode laser procedures (for advanced glaucoma) including a bilateral case, one corneal laceration repair following trauma, a removal of corneal foreign body and a
superficial keratectomy for band keratopathy (scarring of cornea).
We saw just over 200 outpatients. We referred 2 patients to the Eye Unit at Queen Elizabeth Hospital, Blantyre, one for retinal detachment surgery and a baby for bilateral congenital cataract surgery.

Challenges and opportunities
To sustain the work started the single most important intervention is to provide leadership in the department . This may be achieved by the engagement of an ophthalmologist to continue the work started. Precious Kadzongwe our cataract surgeon undergoing training in Tanzania is not back till mid 2024 so an urgent stop gap is necessary. It is essential to secure funding to ensure he completes his training if this hasn’t been done already. With the high demand for eye services in the area the opportunity to deliver a good service not just for cataract surgery but for optical services ought to be taken.
Partnerships with organisations like Sight 2020 Direct will go a long way in supporting cataract surgery activity. We are also currently engaged with ‘One sight Foundation’ to help address refractive errors in Mulanje. This collaboration will help address the provision of Optical services initially for 6 months to promote self-reliance. The sale of glasses will bring in much needed revenue to help keep the unit afloat financially. The appointment of an experienced optometrist to the unit will help facilitate this aim. If this is timed to overlap with the presence of an ophthalmologist this will ensure better provision of services and the smooth running of the department.
Serious consideration should be given to the provision of phacoemulsification cataract services at MMH. If this were implemented it could help bring in much needed revenue to support the department in the long term, It can also serve as a training hub in Malawi where trainees from Blantyre can rotate to the department and receive education in this area. This would be only the second unit in Malawi after Adventist Lilongwe to offer this service.
Summary
The unit in Mulanje has made huge strides and is set to make a big impact on the fight against avoidable blindness not only in Mulanje but in Malawi. With a little more support by appointing 2 more key staff members we should a have a self-supporting sustainable unit within 2 years.
Andrew Feyi-Waboso
